As of 1st April 2022, new Liberty Protection Safeguards (LPS) will be in force. Many people in the UK who lack the mental capacity to consent to care experience deprivation of liberty. This enables care for those with dementia, autism, learning disabilities, etc. Significant court cases were a major factor in changing the Deprivation...
Social Care Trends in 2019: Continued Recruitment Struggles
Recruitment has always been an issue for the care sector and it is likely to endure. The sector forecasts a shortage of 350,000 workers by 2028 assuming no significant changes are made. In reality, slow but steady technology improvements, provided the funding emerges, will chip away at this number. In the short-medium term, though,...
Social Care Trends for 2019: More Focus on Loneliness
2018, as well as an increased emphasis on mental health across all ages, saw numerous campaigns on loneliness among Britain’s older population (and to a lesser extent, in its young people too). Many of those older people who are lonely, of course, are not the types to be on social media campaigning themselves. Change...
Reablement: a brief introduction
Reablement is becoming an increasingly hot topic in the health and social care sector. As budgets continue to come under pressure, reablement offers a way to reduce costs for councils whilst maintaining peoples’ independence. In 2018, we released an ebook that covered the basics of reablement. We have now produced this in a blog...
The NHS Long-Term Plan: What it means for training
The Government published its long-term plan for the NHS this week. We’ve looked at what it means for mandatory, clinical and specialist training for the next decade: Focus on mental health There has been a huge emphasis on mental health in the media and in politics in recent times, and this has carried...
What you need to complete the Care Certificate
The Care Certificate was launched in April 2015. At the time and since, it has been subject to many myths and misconceptions. What is the Care Certificate? What do your staff need to do to be able to complete it? What is the Care Certificate? The Care Certificate is a set of 15 standards...
More than funding needed to change social care
Readers will be well advised to read a very interesting and provocative article in The Spectator on the need for reform in the social care system, concluding the system needs much more than just fresh cash. The article, by James Mumford, who led a review of social care for the Centre for Social Justice,...
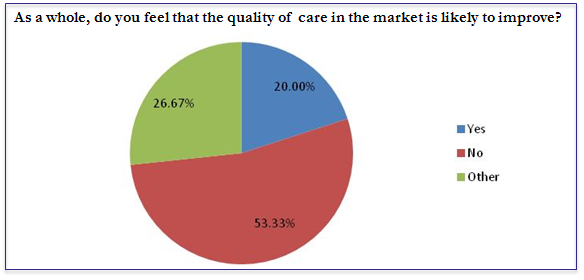
Many pessimistic about the future of care
The results of an Advantage survey for a new report on the Future of Care show that many in the care sector are pessimistic about the future of the sector and the quality of care. The survey asked respondents to rate their optimism about the future of the sector out of 10, with 10 being...
No stop for health and social care integration efforts
The head of NHS England has signalled that there is no intention of ending plans to more closely link the British health and social care systems. A report from the National Audit Office earlier this year suggested that health and social care integration was not being carried out effectively enough to deliver the desired...
New start-up presents new model for care
A new start-up is seeking to let more people with dementia live in their own home by using technology. Adam and Daniel Pike started SuperCarers in response to their own family’s experience with dementia. Their grandmother suffered with the disease, but preferred to stay in her own home. Lacking the finances to pay for...