Readers will be well advised to read a very interesting and provocative article in The Spectator on the need for reform in the social care system, concluding the system needs much more than just fresh cash. The article, by James Mumford, who led a review of social care for the Centre for Social Justice,...
CQC report finds good care in mental health services
Although the media will no doubt focus on the negatives, a new CQC report on the state of care in mental health services has actually uncovered a lot of good news. A study of mental health services conducted between 2014 and 2017 has found that 68% of core services provided by the NHS are...
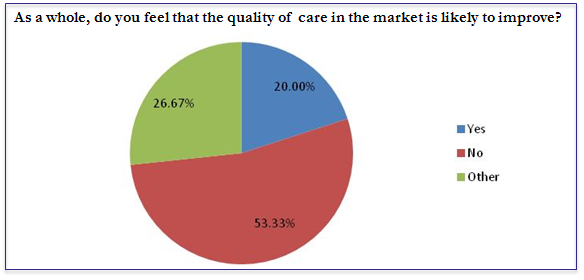
Many pessimistic about the future of care
The results of an Advantage survey for a new report on the Future of Care show that many in the care sector are pessimistic about the future of the sector and the quality of care. The survey asked respondents to rate their optimism about the future of the sector out of 10, with 10 being...
Did you know about Skills for Care’s Leadership Programme?
Skills for Care are ramping up the publicity on their Leadership Programme, which is open to applications. Skills for Care have a raft of leadership programmes (with a discount for members) that many seem unaware of. Although it can be hard to take time out of an organisation, it’s always important to ‘sharpen the...
SCIE makes the case for intermediate care
The Social Institute for Excellence has published a new highlights paper on how intermediate care can deliver better outcomes for people in care. The report has found that effective intermediate care reduces pressure on hospitals and on social care settings. For example, it has found that 72% of people who received intermediate care did...